Recurrent anal sac disease is surprisingly common – and easy to underestimate. It is one of the few chronic conditions in small animal practice that is routinely minimized, often distilled down to a quick “just do their glands” during a busy appointment. Because manual expression typically provides immediate relief, it is understandable that owners – and sometimes even clinicians – assume the problem begins and ends with mechanical emptying. Maybe add a little fiber, consider a probiotic, and see the dog next month.
Meagan Painter, DVM, DACVD
Board-Certified Veterinary Dermatologist®
Founder, The Allergic Dog™ (www.theallergicdog.com)
November 2025
When I was in my dermatology residency, I didn’t learn much about anal sacs. And, this issue certainly was not a focus for me in my practice as a dermatologist.
Well, that all changed when I had a case referred to me for anal sacculitis. Sadie, a Vizsla, had seen several veterinarians for her moderate to severe perianal pruritus, leakage, and scooting. Before referring to a surgeon, they recommended a dermatologist. And…I wasn’t really sure what I could do to help her.
So, I read a lot – I talked to other doctors – and I grew as a clinician. And, in the end, I was able to help Sadie in a lasting way. I hope sharing this case and this information helps you, too!
Case Presentation
Sadie was referred to our dermatology service for “ongoing anal gland issues” that had become a fixture in her household routine. She scooted daily, often multiple times per day, and licked her perianal region with an intensity her owners described as “constant.” Her anal sacs had been expressed every three to four weeks for more than a year, performed alternately by the groomer and the primary veterinarian. She received lokivetmab on roughly the same interval, with variable benefit. Her owners had added various “gut health” chews they found online. Stool quality fluctuated between formed and soft, and general pruritus was described as mild, with a PVAS of 2–3/10 outside of her perianal flare-ups. She was described as a somewhat picky eater. She had mild atopic symptoms, but this was significantly more severe.
When I saw Sadie, she was wearing a diaper and had bloody anal sac contents leaking from her anus. It was really sad to see – she was clearly miserable, and so was her family.
Perianal examination showed mild lichenification of the anus, moderate salivary staining of the haired skin surrounding the anus, and no external swelling or draining tracts. Rectal palpation was within normal limits. The right sac expressed easily and was essentially “leaky”. The left required more manipulation, and seemed to bother her more. The secretions were thin and watery to darker brown, with a bloody tinge. Her overall dermatologic exam revealed mild interdigital erythema, ceruminous otitis, and subtle erythema of the concave pinnae. Otherwise, Sadie appeared healthy and comfortable.
Cases like Sadie’s raise important clinical questions. Is the problem infection, inflammation, or both? What diagnostics are truly useful? What pathogenesis explains these signs? And most importantly: what interventions will make a meaningful difference?
Understanding What We’re Seeing
Anal sac disease exists along a clinical spectrum, from impaction to inflammatory sacculitis to true abscessation. Sadie showed no signs of abscess. She had no evidence of cellulitis, pain, systemic illness, or tissue involvement beyond the sac. Her sacs were not markedly distended, making a diagnosis of anal sac impaction unlikely. Instead, the chronic perianal pruritus signs, accompanied by variable anal sac contents that had started to become more hemorrhagic in nature, pointed clearly toward a chronic inflammatory problem involving the anal sacs.
This is where many dogs live clinically – and where many get stuck. The sacs become the focus of repeated interventions, but the underlying inflammatory contributors remain unaddressed. And, worse, some are treated with antibiotics which rarely solve the problem.
What Drives These Signs?
When we are looking to understand the root cause to an anal sac problem in dogs, we have to think of the three ways that anal sacs can become problematic.
The first – abscess. This often results from incomplete emptying with secondary infection that leads to rupture of the sac, cellulitis, and other systemic sequelae. This is an infectious issue, and often happens in dogs without underlying predisposing causes. This is not the focus of this article, but I will say that antimicrobial stewardship and consideration for the role that inflammation plays in these cases is essential.
Second – impaction. This often results from incomplete emptying as a result of chronic soft or variable stool quality. Dogs with impaction may or may not have active clinical signs of perianal pruritus. But, if they do, and they have stool issues – fix the stool issues to see if the sacs improve. They could be a bystander, impacted (see what I did there…!) by chronic enteropathy.
Third – sacculitis. As the name implies, this is an inflammatory problem of the anal sacs. In most cases, allergic inflammation alters perianal sensitivity, alters secretion viscosity, impacts ductal function, and creates a chronic cycle of lick/scoot/express/repeat. These dogs do not have infection, they have inflammation. And, most of these dogs are allergic dogs – and their anal sacs are one of the many ways that they manifest inflammation and itch.
Oh, also, cats. I am not talking about cats in this article because, luckily, this problem is not a common one for this species – likely due to some anatomic and secretion differences. However, the spectrum of impaction, sacculitis, and abscess are similar in this species.
Diagnostics: What Matters and What Doesn’t
When faced with a dog like Sadie, who has moderate to severe anal sacculitis, clinicians naturally consider whether additional diagnostic testing might clarify the picture. Should you do cytology? Bacterial culture and sensitivity? Other tests?
The answer – no.
Anal sacculitis cases rarely progress to anal sac abscess cases. This is an inflammatory problem, not an infectious one. Both healthy and diseased anal sacs contain bacteria, and differentiating normal flora from dysbiosis from true infection can be difficult without clinical context. Chasing culture results also risks focusing on organisms rather than inflammation. Many chronic cases like Sadie’s have received multiple antibiotic courses – often from three or more antimicrobial classes – without any lasting improvement. This creates unnecessary exposure and contributes greatly to antimicrobial resistance. If you learn one thing from this article, it is to stop treating your anal sacculitis cases with systemic antibiotics. There are more effective strategies.
Cytology of sac contents is similarly nonspecific. Neutrophils, variable bacteria, and debris appear across all categories of anal sac disease and cannot guide clinical outcome or diagnosis.
Instead, diagnostics should focus on the dog’s global inflammatory context: dermatologic examination, allergy assessment, dietary and GI evaluation, and careful review of chronicity and recurrence. In other words, this is a diagnosis rooted in your clinical skills as a historian. Does this case fit the picture of an allergic dog with anal sac inflammation? Does this case fit the picture of a dog with a diet-responsive enteropathy with anal sac impaction? Does this case fit the picture of a food allergic dog with anal sac impaction and sacculitis? The more you ask these questions, the more you will likely say yes to at least one of these questions.
Therapeutic Plan
So, let’s talk about what we can do about it – beyond expression.
Management for dogs like Sadie requires both systemic and local strategies.
Systemically, optimizing allergic disease management is essential. Sadie’s owners began a strict diagnostic diet trial with a hydrolyzed prescription food. This was coached in such a way to be administered to a diagnostic standard for best results. Within a few days, her stool quality had normalized and her picky eating behavior improved. This was considered “root cause work” which addressed the systemic source of her inflammation. Had her diet trial been negative, consideration for allergen testing with the explicit purpose of starting allergen-specific immunotherapy could have been considered. Remember, allergen testing is non-diagnostic. And, results from “food allergen” IgE tests cannot be used to make a diagnosis of food allergy in dogs; the diagnostic diet trial remains the gold standard test.
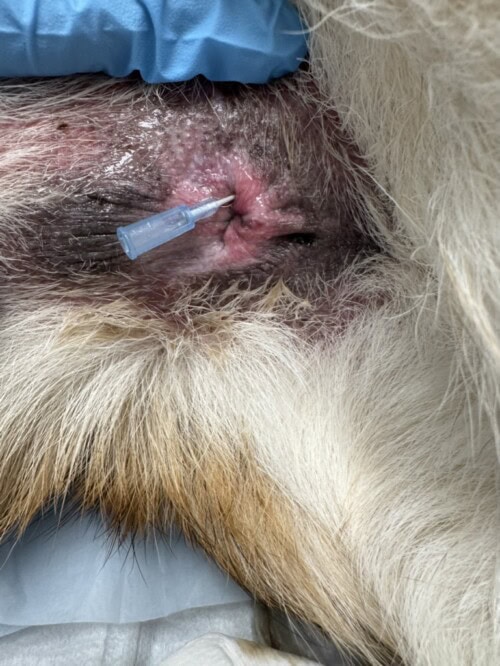
Locally, her sacculitis was addressed with a sedated anal sac lavage and corticosteroid infusion procedure. This procedure is highly effective for sacculitis cases when performed with proper technique. The goal is to reduce active inflammation by applying steroids locally. To perform this procedure, the patient is placed laterally or sternally (author prefers laterally). The anal sac duct is identified, and a catheter stylet is gently introduced into the duct to the level of the anal sac. I utilize a product like Animax® or Mometamax® during my infusions. The most important ingredient in the product is the steroid, so infusions with antibiotic-only creams or gels are discouraged. Remember, this is an inflammatory problem first. The infusion is repeated on both sides. A detailed description is available in the literature and is covered comprehensively in Beyond Expression™, the course I teach through The Allergic Dog™.
Photo shows a 22g catheter stylet (needle removed) inserted into the left anal sac duct.
Outcome
At her four-week recheck, Sadie’s owner reported complete resolution of scooting and a dramatic decrease in perianal licking. Her stool consistency remained stable, her general comfort improved, and her perianal staining was beginning to fade. A single infusion procedure was useful for her, as it is for most dogs described in the literature. Sadie maintained control of her sacculitis at follow-up visits while continuing her diet and supportive treatments for other allergic symptoms (occasional lokivetmab).
Clinical Reflections
Sadie’s case illustrates a pattern many clinicians will recognize: a dog that requires repeated expression every few weeks, and you always kind of wonder if there is more that you could do. Just remember – the sacs are not the core problem – the inflammation is. Sacculitis and/or anal sac impaction is rarely isolated; more often, it is an extension of allergic or gastrointestinal disease. When we shift our focus away from cultures, repetitive expression, and unnecessary antibiotics – and instead assess the dog’s global inflammatory context – diagnostic clarity improves and clinical outcomes follow.
Anal sac infusion therapy can be an excellent adjunct in cases of chronic anal sacculitis. When paired with improved allergic control and optimized stool consistency, it provides durable, meaningful relief for many patients.
Closing Thoughts
Anal sac disease deserves more attention than the familiar “just do their glands” routine allows. Reframing these cases through an Inflammation First™ lens offers veterinarians a clearer diagnostic pathway and significantly better therapeutic outcomes. This also improves our overall professional commitment to antimicrobial stewardship. For clinicians seeking detailed, case-based instruction – including infusion technique, communication strategies, and management algorithms – I offer a comprehensive course through The Allergic Dog™:
https://www.theallergicdog.com/anal-glands
I hope that you enjoyed this article, and hot take on a common problem. I love to support veterinarians with practical, evidence-based guidance that improves the lives of allergic dogs!
References
Lundberg A, Koch SN, Torres SMF. Local treatment for canine anal sacculitis: A retrospective study of 33 dogs. Vet Dermatol. 2022;33(5):426-434. doi:10.1111/vde.13102
Hvitman-Graflund K, Sparks T, Varjonen K. A retrospective study of treatment, outcome, recurrence and concurrent diseases in 190 dogs with anal sacculitis. Vet Dermatol. 2023;34(6):576-585. doi:10.1111/vde.13205
C Bergeron C, Costa MC, Segura M, de Souza LB, Bleuzé M, Sauvé F. Bacterial microbiota and proinflammatory cytokines in the anal sacs of treated and untreated atopic dogs: Comparison with a healthy control group. PLoS One. 2024;19(5):e0298361. Published 2024 May 30. doi:10.1371/journal.pone.0298361
van Duijkeren E. Disease conditions of canine anal sacs. J Small Anim Pract. 1995;36(1):12-16. doi:10.1111/j.1748-5827.1995.tb02756.x
O’Neill DG, Hendricks A, Phillips JA, Brodbelt DC, Church DB, Loeffler A. Non-neoplastic anal sac disorders in UK dogs: Epidemiology and management aspects of a research-neglected syndrome. Vet Rec. 2021;189(2):e203. doi:10.1002/vetr.203