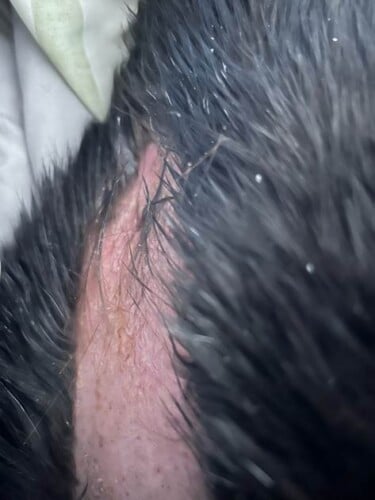
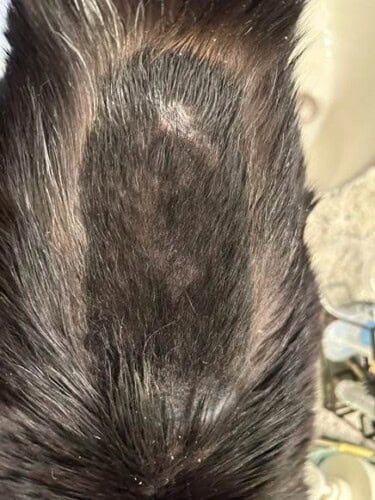
Pixie” is a 5y FS DSH who presented for a history of well-demarcated alopecia on the dorsum of more than a year’s duration. The affected area of the dorsum is not especially pruritic that owner has noticed; Pixie occasionally licks her dorsum, but can only reach about the caudal third of the affected area with her tongue when grooming herself.
Curtis Plowgian
DVM, DACVD, ADC Indianapolis
March 2026
History
No other lesions have developed anywhere except for the back. Problems have been year-round and non-seasonal. Owner has 2 other cats that are unaffected, and all 3 cats are on Revolution Plus monthly, and owner has 2 dogs who are unaffected and are on Revolution monthly. PDVM tried treating Pixie with oral liquid prednisolone, but this was discontinued after 2 weeks due to perceived lack of effect. Owner also tried transdermal Prozac on the pinnae for 3 months, this stopped total body licking but no benefit was noted on the dorsum, and this was stopped because it made Pixie hide from owner. Currently on Royal Canin HP strictly since January, no perceived difference. One treatment that helped the sore on the caudal aspect of the lesion was a Convenia injection, and this has been repeated twice. No current meds for the skin, but owner is applying topical Vitamin E to help with drying, cracking, and flaking. Owner also using Neosporin SID on current sore.
Physical Exam
There is a large, well-demarcated region of smooth erythematous to hyperpigmented alopecia on the throacolumbar dorsum, with a small cluster of sores/ulcers on the caudal third of the region, and the cranial margins of the thoracic dorsum have much less hyperpigmentation, but moderate to marked scale/crust present on the surface of the skin.
Diagnostics
Cytology of different areas on the dorsal lesion revealed TNTC WBCs and streaming but no obvious organisms (sore), TNTC keratinocytes but no organisms (cranial scale/crust)
Assessment
Well demarcated dorsal alopecia, r/o alopecia areata vs pseudopelade vs thermal burn vs other local trauma vs vasculitis
Overgrooming, suspect stress/behavioral over allergic (since better response to prozac than pred)
Treatment Plan
Discussed with owner that without a more precise idea of what was causing the alopecia, treatment would be difficult. Discussed the possibility of a thermal burn or other physical or chemical injury, but owner was certain that no such incident had occurred prior to the onset of the lesion. To investigate other underlying causes of the alopecia and lesions, a 2-site biopsy was performed (taking two 8mm punches, one from a scaly area of the cranial dorsum, and one from the more ulcerated area of the caudal dorsum). Medical therapies were put on hold pending biopsy results. Biopsy results came back in 2 weeks, and were reported as follows:
Diagnosis
Haired skin: moderate regionally extensive fibrosis/fibroplasia with adnexal loss, chronic lymphoplasmacytic perivascular dermatitis, epidermal hyperplasia, hyperkeratosis and erosions Haired skin: moderate diffuse epidermal, follicular and dermal atrophy with adnexal loss and mineralization
Comments
Both samples contain slightly different findings. One has chronic inflammation with regional fibrosis and adnexal loss. The other section has generalized epidermal, follicular and adnexal atrophy. The underlying etiology is not apparent on histology exam, but chronic smoldering vasculitis or previous thermal injury with/without self-trauma (itch, pain, neuropathic) are considerations. An endocrinopathy was also considered due to the generalized atrophy, however, this is considered less likely given the focal nature. Clinical correlation is needed.
Given the lack of clinical correlation with an endocrinopathy, chronic nature of the lesion, and lack of immediate pruritus, pentoxifylline was started at 15mg/kg BID and topical tacrolimus was started at BID application for 2 weeks, then SID applications until recheck exam.
Follow-up
4 weeks after the above therapies were started, the owner sent an email saying that she was seeing marked improvement on Pixie’s dorsum. While the hair hadn’t fully grown in, owner was seeing more hair regrowth than at any point in the last year, and there were no signs of obvious pruritus or overgrooming, and no noted adverse effects to every of the medications.
8 weeks after the onset of therapies, the owner sent an email stating that hair had completely regrown, and Pixie seemed “back to normal”. Owner was so happy with Pixie’s progress that she discontinued the medications, and cancelled her upcoming recheck examination. In the last 2 months, Pixie has been lost to follow up, but there have been no reports from owner about any signs of relapse or return of overgrooming or lesions.
Discussion
This was an interesting case, in that clinical resolution of lesions was reached without a definitive diagnosis being made. Based on a combination of the biopsy findings and response to medical management, the most likely diagnosis in this case was some form of vasculitis or ischemic dermatopathy. Vasculitis or ischemic dermatopathies can be very interesting dermatologic syndromes, as they can have a variety of clinical presentations and underlying causes1. In dogs, toy and miniature breeds are more commonly affected, with Chihuahuas, Yorkshire Terriers, and Miniature Poodles being overrepresented in some studies2. Many cases are vaccine associated, but other causes can include insect envenomation, rickettsial and other tick-borne illness, food allergies, medication reactions, other hypersensitivity reactions, frostbite, other physical or thermal trauma and in some cases no inciting cause is found (idiopathic)1,2.
Treatment usually involves avoidance of the underlying or inciting cause (if one is found), and supportive or symptomatic therapy is usually provided by a combination of medications aimed at reducing immune-mediated inflammation and improving circulation/perfusion. Pentoxifylline is particularly helpful in these circumstances given its anti-inflammatory effects and its effects increasing erythrocyte flexibility and reducing blood viscosity3. In milder cases, supplements and nutraceuticals such as Vitamin E and Omega 3 fatty acids can be helpful, or these can be added adjunctively to maintenance medications. In more severe cases, anti-inflammatory medications such as doxycycline and niacinamide, cyclosporine, tacrolimus, glucocorticoids are used, and in more severe cases, hydroxychloroquine, azathioprine, and mycophenolate have been used2.
Prognosis can be highly variable, from some cases resolving without the need for continued medications (usually if inciting trigger can be identified and removed), to some cases needing lifelong medications. In some severe cases, patients may be euthanized due to poor control of their disease or adverse effects from their medications2.
In this case, the author’s first clinical suspicion was of physical or thermal trauma (the lesion resembled a heating pad burn), but it is curious that there was no recovery or healing noted in over a year, and that new sores and ulcers continued to appear on the surface of the dorsum so long after the onset of the inciting injury or disease. Histopathology of the affected skin seemed to support an initial thermal injury, with additional findings consistent with a chronic vasculitis or ischemic dermatopathy. Given the lack of progression of disease over a year, the clinical decision was made to treat conservatively with pentoxifylline and tacrolimus.
Pentoxifylline can take 1-2 weeks (or more) to reach therapeutic effect3; in the author’s experience it can often take 4-8 weeks. Tacrolimus was added to speed improvement, but both of these drugs are typically well-tolerated with few adverse effects. While Pixie took 8 weeks to reach full hair regrowth, the skin appeared to be healing with partial hair regrowth 4 weeks prior to that per the owner’s photo update. Given that no inciting trigger was definitively identified, it is impossible to predict long-term prognosis or likelihood of relapse at this point, but given that there has been no relapse so far despite discontinuation of medications, there is room for optimism that the inciting cause was a one-time event such as a thermal injury that will not cause recurrent or lifelong disease.
References
Miller WH, Griffin CE, Campbell KL. Muller and Kirk’s Small Animal Dermatology. 7th Philadelphia, PA: Saunders, 2013; 479-488.
Backel, KA, et al. Canine ischaemic dermatopathy: a retrospective study of 177 cases (2005–2016). Vet Dermatol 2019; 30:5, 403-e122.
Plumb, DC. Plumb’s Veterinary Drug Handbook, Eighth Edition. Ames, IA: Wiley-Blackwell, 2015; 836-838.